One of the biggest issues in rural health care is the lack of health care facilities. Many rural areas don’t have enough doctors or hospitals and appropriate care is often far away. This means they may not be able to see a doctor or get lifesaving, emergency treatment quickly when they need it. Rural areas also struggle to keep doctors, nurses and specialists due to lower salaries and the social and professional isolation of working remotely.
Financial concerns also are challenges in rural health care, so advanced equipment and services are often not easily available at rural hospitals, lowering the level of health care offered to residents. Limited resource access and shortages leave patients with fewer options for treatment.
 Rural hospitals are in danger of closing
Rural hospitals are in danger of closing
Small hospitals can struggle financially because they don’t have enough patients to cover their operating costs. Often, they depend on government grants and fundraising to stay afloat and this income source can be unreliable. Since 2010, more than 180 rural hospitals in the U.S. have closed and more are predicted to follow. Government insurance programs, like Medicare and Medicaid, are common revenue sources but these programs don’t pay enough to cover all the costs of running a hospital, haven’t kept pace with the inflation rate since the 2000s and are currently being drastically reduced. This financial strain can make it difficult for these hospitals to stay open and serve rural communities.
When a rural hospital closes, people in that area must travel even farther to get medical care. This can be especially dangerous for people who need emergency care or have serious medical conditions. The closure of these hospitals adds more pressure on other nearby hospitals, making it harder for everyone to get the help they need.
Bridging the gap between remote hospitals and urban health care resources
Solving the rural health care crisis requires improving the connection between rural hospitals and urban health care systems. Telemedicine can be a solution allowing for access to doctors for routine care. Access to specialists not available in rural areas is a benefit of telemedicine as well and is more cost effective than having to travel long distances for care.
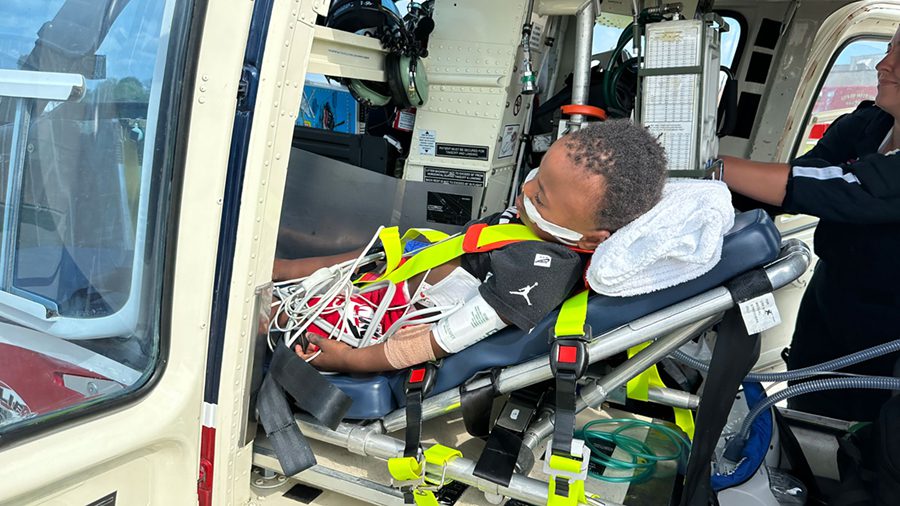
Creating partnerships between rural hospitals and larger urban hospitals can improve access for residents. This will help rural hospitals provide better care by augmenting the availability of needed equipment and services. Additionally, improving transportation options can help rural residents get to health care facilities more quickly, especially in emergency situations. Air ambulances are often used in critical medical need cases when time is of the essence. Routine care transportation for those unable to drive can also improve health outcomes for rural patients.
Posted in: Safety
Comment Policy: All viewpoints are welcome, but comments should remain relevant. Personal attacks, profanity, and aggressive behavior are not allowed. No spam, advertising, or promoting of products/services. Please, only use your real name and limit the amount of links submitted in your comment.
You Might Also Like...

Staying Safe on Social Media – Eight Ways to Protect Your Kids
Like it or not, social media is an important part of our children’s lives. By the time they are teenagers, 95% of kids have used it and 45% admit to […]

Building a Fire-Resilient North State
Wildfire and its aftermath are rapidly becoming a part of everyday life in the western United States. The 2018 Carr and Camp fires, the 2020 August Complex fire and the […]

Women’s Business Center Helps North State Businesses Find & Navigate Disaster Recovery Resources
Between fires, droughts and a global pandemic, Northern California communities have been through many years of disasters and disaster recovery. At this point in time, there is not a person […]

Safety and Security in the North State
Thousands of dedicated law enforcement, fire and first responder personnel throughout the North State work hard every day to respond to emergencies and do their best to protect and serve […]

 Rural hospitals are in danger of closing
Rural hospitals are in danger of closing
