The history of school nursing reflects changes as vast as those in any other medical profession. It began with a single focus: keeping children in school. Today, nurses are responsible for more tasks than one can count on 10 fingers.


The model Lillian initiated was to treat children’s disorders at school and return them to class. By the 1950s and ‘60s, with better sanitary conditions and the development of vaccines and antibiotics, most epidemics had been abolished. School nursing began to shift from a model of treating disease within schools, to health education and the prevention of illnesses.
During that same era, new health and welfare programs emerged. The school nurse’s role expanded, and she recruited assistance from others in the educational system, as well as parents. Even students became involved in their own welfare. The 1970s brought further changes, including an extension of services to combat increases of drug-abuse related disorders, teenage pregnancy, and sexually transmitted diseases. The 1975 passage of the Education for All Handicapped Children Act required that all children with physical and mental disabilities have access to free and appropriate education in the least restrictive educational setting. As schools began complying with the mandate, school nurses’ duties increased to an almost overwhelming degree.
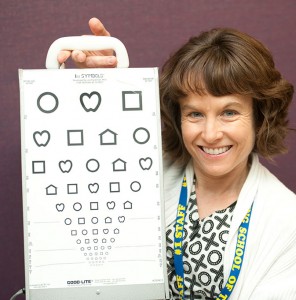

District and county school budget cuts have translated into fewer health services, while school nurse caseloads along with the number of schools she serves has increased.
Teresa Evans, school nurse for Butte County Office of Education, works in nine schools, providing for special education students from preschool through age 22. Her caseload includes children with severe intellectual, physical and/or emotional challenges, as well as those with severe medical conditions. She serves children in the district’s autism program and its deaf and hard-of-hearing program.
Kara Jones, school nurse for the North State Charter Joint Partnership Agreement (JPA), works with charter schools in the Redding area serving differently abled children mainstreamed into regular school classrooms. While some of her students don’t exhibit severe special needs, others do. Her caseload includes children with cerebral palsy, seizures, diabetes, vision and hearing losses, and serious allergies.
As part of their jobs, these two nurses conduct vision, hearing and dental screenings. They talk to parents about their findings and provide parent education. They write health protocols for teachers and administrators to follow, as well as provide staff trainings on how to handle health issues, and how to use and manage health equipment such as the EpiPen (for students allergic to bee stings), wheel chairs, and apparatuses required for tube feeding of severely challenged students.


Your head may be swimming with the number of tasks a school nurse is required to perform beyond taking care of student injuries or illnesses during the day. Yet most of them carry out the functions of their jobs with grace and patience. “I like the diversity of my job,” says Jones. “I enjoy going from school to school and interfacing with both adults and children. I’m always learning new information.”
Evans likes the power of teamwork. “It takes a team working together to help the children and families. It is gratifying when we can see the growth of our students as a result of our teamwork and parent involvement.”
What are some challenges that school nurses face? Evans says, “Many of the parents I work with live below the poverty line. Often they don’t have the resources to take care of their own physical and emotional needs, so they can’t be as attentive to the needs of their children.”
Jones says, “We have a huge volume of students with serious health needs entering our mainstream classrooms. Teachers feel apprehensive about how to serve them, and nurses often feel they cannot adequately meet the needs of all the children and staff as well as they would like.”
When a kindergarten child was asked what her school nurse does, she replied, “She looks at your eyes, ears, mouth and nose.” Many adults also think this is a school nurse’s role. Unless their child has a special health need, most people are unaware of the major responsibility a school nurse has in the school system today.
Posted in: Community, Education, Health & Nutrition
Comment Policy: All viewpoints are welcome, but comments should remain relevant. Personal attacks, profanity, and aggressive behavior are not allowed. No spam, advertising, or promoting of products/services. Please, only use your real name and limit the amount of links submitted in your comment.
You Might Also Like...

Great Ways Dads are Different
There is no denying that there are differences between how moms and dads parent their kids. Just because dads may do things differently than moms doesn’t mean their parenting style […]

Uplifting “Tails” of Pets Loved, Lost and Found
For true pet lovers, our dogs, cats, turtles and even chinchillas are deeply loved. We can’t imagine our family circle complete without them. During the 2018 Carr Fire that burned […]

Lying or Pretending? Teaching Kids to Tell the Truth
Somewhere around the age of three, when children begin to understand parents may not know what they actually did or didn’t do, your precious little angel may begin to tell […]

On Pins And Needles – The Benefits Of Acupuncture
For a woman who admits being extremely afraid of needles, Patti Furnari is a huge fan of acupuncture. Having dealt with the debilitating pain of migraines for over 25 years, […]


